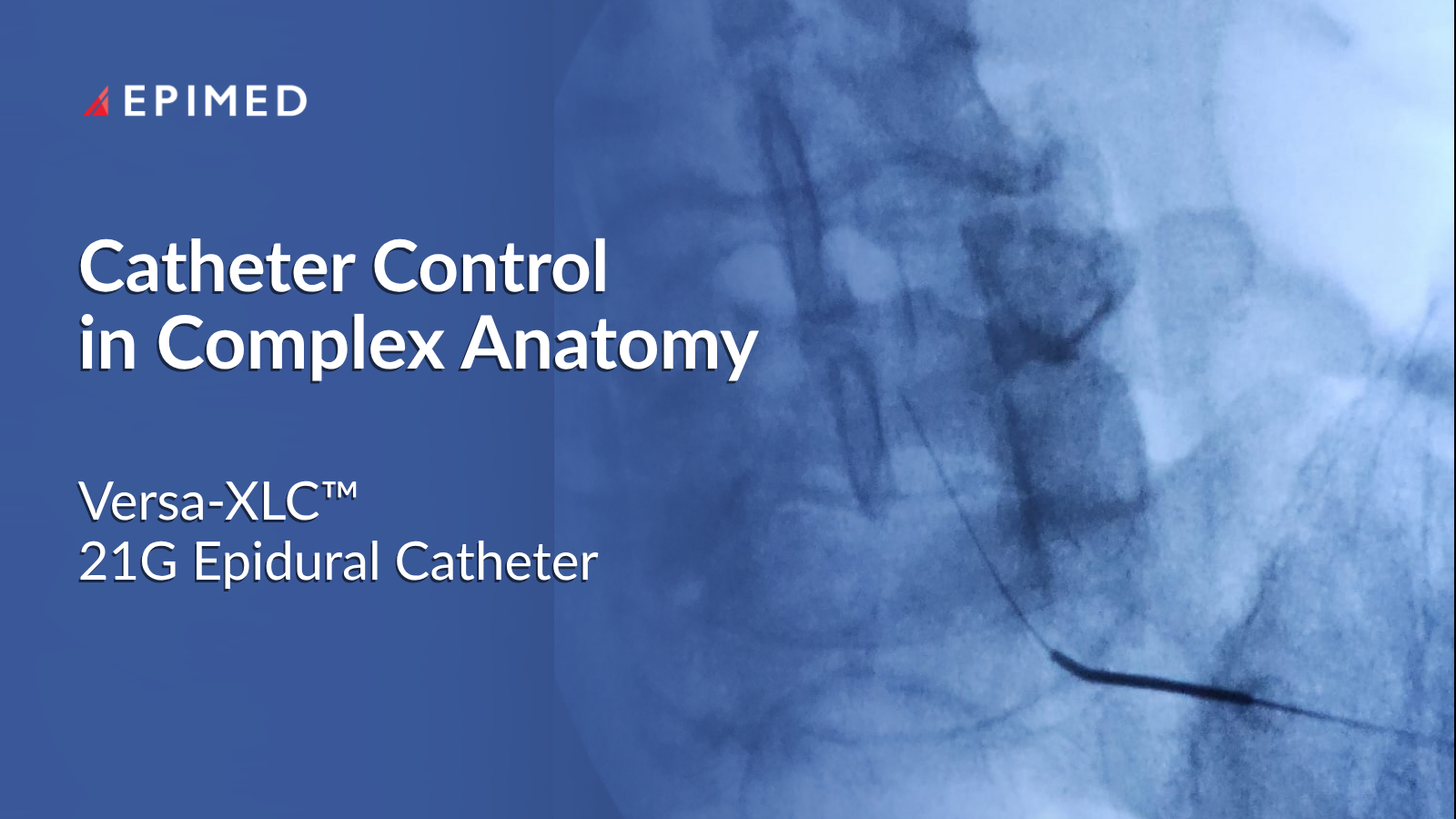
Variability in outcomes often stems from challenges such as limited control during navigation, poor fluoroscopic visibility, suboptimal medication distribution, and difficulty managing complex or scarred anatomy. These factors can directly impact procedural efficiency and therapeutic success.
Variability in outcomes is often linked to:
- Limited control during navigation
- Reduced fluoroscopic visibility
- Suboptimal medication distribution
- Challenges in complex or scarred anatomy
These factors can directly impact both procedural efficiency and therapeutic results.
Why Catheter Behavior Matters
In straightforward cases, standard catheter designs may be sufficient. However, in complex anatomy where adhesions, narrowing, or anatomical variations are present, catheter performance becomes an important factor.
Control, responsiveness, and visibility are essential for:
- Reaching the intended target
- Adjusting trajectory
- Delivering therapy accurately
When catheter behavior is limited, procedural adaptability is also limited.
Control vs. Flexibility: A Clinical Balance
Catheter design inherently involves a balance between flexibility and control.
More flexible catheters can navigate with ease but may lack the directional stability needed in challenging cases. In contrast, increased stiffness can enhance steering and responsiveness but may introduce slight resistance during advancement.
Designed for experienced users, the Versa-XLC™ supports a more controlled approach to catheter advancement without sacrificing procedural intent.
Catheter design involves a balance between flexibility and control.
- More flexible catheters may navigate easily but offer less directional stability
- Stiffer catheters may provide improved steering and responsiveness, particularly in challenging cases
This comes with a clinical trade-off: Greater control may introduce a slightly increased resistance during advancement or injection—an expected characteristic for experienced users.
Design Considerations in 21G Epidural Catheters
In 21G epidural procedures, catheter behavior becomes particularly important.
Smaller gauge catheters require a higher level of procedural control, including:
- Precise navigation within confined anatomical spaces
- Controlled and predictable advancement
- Clear visualization under fluoroscopy
In these settings, design characteristics such as stiffness, tip configuration, and radiopacity can significantly influence catheter performance and overall procedural efficiency.
Why Distribution Matters
Effective therapy depends not only on reaching the target, but also on how medication is distributed within the epidural space.
Inconsistent or limited distribution may affect therapeutic response, particularly in cases involving:
- Nerve irritation
- Inflammatory processes
- Epidural adhesions
Catheter design can play a role in facilitating more controlled and predictable spread, especially when lateral distribution is required.
The Importance of Visibility
Fluoroscopic visualization is critical throughout epidural procedures.
Limited visibility can affect:
- Position confirmation
- Trajectory adjustment
- Confidence during navigation
Enhanced radiopacity allows physicians to track catheter position more clearly in real time—particularly in complex cases.
Controlled Navigation in Complex Anatomy: The Role of the Versa-XLC™ 21G Epidural Catheter

The Versa-XLC™ is designed to support controlled catheter navigation in challenging anatomical environments. Design elements supporting control include:
- XL stylet extending to the distal tip, contributing to a stiffer profile and improved directional control
- Enhanced radiopacity for precise fluoroscopic visualization
- Closed tip with three side ports supporting lateral medication delivery
- 1:1 torque response for predictable and controlled advancement
Clinical Use Considerations
- The Versa-XLC™ is not intended for every procedure.
- It is designed for physicians who require: greater control in complex anatomy, improved visualization, more responsive catheter behavior
FAQ
Q1: Why does catheter stiffness matter in epidural procedures?
Catheter stiffness influences directional control during navigation. A stiffer catheter can provide improved steering and stability, particularly in complex or narrowed anatomical spaces. However, increased stiffness may also result in slightly greater resistance during advancement or injection.
Q2: How does catheter design impact medication delivery?
Catheter design affects how medication is distributed within the epidural space. Features such as side ports can support lateral distribution, which may improve coverage of the targeted area, especially in cases involving inflammation or adhesions.
Q3: Why is fluoroscopic visibility important for epidural catheters?
Fluoroscopic visibility allows physicians to track catheter position in real time. Improved radiopacity can enhance placement accuracy, support trajectory adjustments, and increase confidence during navigation, particularly in complex procedures.
Q4: How does the Versa-XLC™ epidural catheter differ from more flexible catheters?
The Versa-XLC™ is designed with increased stiffness and a stylet extending to the distal tip, which supports improved directional control.
Compared to more flexible catheters, it provides a more controlled response during navigation, particularly in complex anatomical environments.
Q5: Is the Versa-XLC™ suitable for all epidural procedures?
No, the Versa-XLC™ is not intended for all procedures. It is designed for cases where enhanced control, visualization, and responsiveness are required. Catheter selection should always be based on clinical judgment and procedural context.
 Sign in
Sign in
 Create Account
Create Account